What is a veterinarian?
A veterinary physician, colloquially called a vet, shortened from veterinarian or veterinary surgeon, is a professional who practices veterinary medicine by treating disease, disorder, and injury in non-human animals.
.Most vets work in clinical settings, treating animals directly. These vets may be involved in a general practice, treating animals of all types; may be specialised in a specific group of animals such as companion animals, livestock, zoo animals or horses; or may specialise in a narrow medical discipline such as surgery, dermatology or internal medicine.
Vets are primarily required to treat disease, disorder or injury in animals, which includes diagnosis, treatment and aftercare. The scope of practice, speciality and experience of the individual vets will dictate exactly what interventions they perform, but most will perform surgery (of differing complexity).Unlike in adult human medicine, vets must rely on clinical signs, as animals are unable to vocalise symptoms as a human would (and in that respect is similar to medicine on human children). In some cases, owners may be able to provide a medical history and the vet can combine this information along with observations, and the results of pertinent diagnostic tests such as x-rays, CT scans, blood tests, urinalysis or other diagnostics.As with human medicine, much veterinary work is concerned with prophylactic treatment, in order to prevent problems occurring in the future. Common interventions include vaccination against common animal illnesses, such as distemper or rabies. This may also involve being involved in owner education so as to avoid future medical or behavioural issues. Unlike in most human medicine, vets will often consider the appropriateness of euthanasia ("putting to sleep") if a condition is likely to leave the animal in pain or with a poor quality of life.
.Most vets work in clinical settings, treating animals directly. These vets may be involved in a general practice, treating animals of all types; may be specialised in a specific group of animals such as companion animals, livestock, zoo animals or horses; or may specialise in a narrow medical discipline such as surgery, dermatology or internal medicine.
Vets are primarily required to treat disease, disorder or injury in animals, which includes diagnosis, treatment and aftercare. The scope of practice, speciality and experience of the individual vets will dictate exactly what interventions they perform, but most will perform surgery (of differing complexity).Unlike in adult human medicine, vets must rely on clinical signs, as animals are unable to vocalise symptoms as a human would (and in that respect is similar to medicine on human children). In some cases, owners may be able to provide a medical history and the vet can combine this information along with observations, and the results of pertinent diagnostic tests such as x-rays, CT scans, blood tests, urinalysis or other diagnostics.As with human medicine, much veterinary work is concerned with prophylactic treatment, in order to prevent problems occurring in the future. Common interventions include vaccination against common animal illnesses, such as distemper or rabies. This may also involve being involved in owner education so as to avoid future medical or behavioural issues. Unlike in most human medicine, vets will often consider the appropriateness of euthanasia ("putting to sleep") if a condition is likely to leave the animal in pain or with a poor quality of life.
Equine Infectious Anemia (EIA)
Equine infectious anemia or equine infectious anaemia (EIA), also known by horsemen as swamp fever, is a horse disease caused by a retrovirus and transmitted by bloodsucking insects. The virus is endemic in the Americas, parts of Europe, the Middle and Far East, Russia, and South Africa. The virus is a lentivirus, like human immunodeficiency virus (HIV). Like HIV, EIA can be transmitted through blood, saliva, milk, and body secretions. Transmission is primarily through biting flies, such as the horse-fly and deer-fly. The virus survives up to 4 hours in the carrier. Contaminated surgical equipment and recycled needles and syringes, and bits can transmit the disease. Mares can transmit the disease to their foals via the placenta. The risk of transmitting the disease is greatest when an infected horse is ill, as the blood levels of the virus are then highest.
Acute: The acute form is a sudden onset of the disease at full-force. Symptoms include high fever, anemia (due to the breakdown of red blood cells), weakness, swelling of the lower abdomen and legs, weak pulse, and irregular heartbeat. The horse may die suddenly.
Subacute: A slower, less severe progression of the disease. Symptoms include recurrent fever, weight loss, an enlarged spleen (felt during a rectal examination), anemia, and swelling of the lower chest, abdominal wall, penile sheath, scrotum, and legs.
Chronic: Horse tires easily and is unsuitable for work. May have a recurrent fever and anemia, may relapse to the subacute or acute form even several years after the original attack.
There are currently no statistics available on mortality of EIA. No statistics are available of horses actually dying of acute forms.A horse may also not appear to have any symptoms, yet still tests positive for EIA antibodies. This horse can still pass on the disease. According to most veterinarians, horses diagnosed EIA positive are usually not showing any sign of sickness or disease.EIA may cause abortion in pregnant mares. This may occur at any time during the pregnancy if there is a relapse when the virus enters the blood. Most infected mares will abort, however some give birth to healthy foals. Foals are not necessarily infected.
Acute: The acute form is a sudden onset of the disease at full-force. Symptoms include high fever, anemia (due to the breakdown of red blood cells), weakness, swelling of the lower abdomen and legs, weak pulse, and irregular heartbeat. The horse may die suddenly.
Subacute: A slower, less severe progression of the disease. Symptoms include recurrent fever, weight loss, an enlarged spleen (felt during a rectal examination), anemia, and swelling of the lower chest, abdominal wall, penile sheath, scrotum, and legs.
Chronic: Horse tires easily and is unsuitable for work. May have a recurrent fever and anemia, may relapse to the subacute or acute form even several years after the original attack.
There are currently no statistics available on mortality of EIA. No statistics are available of horses actually dying of acute forms.A horse may also not appear to have any symptoms, yet still tests positive for EIA antibodies. This horse can still pass on the disease. According to most veterinarians, horses diagnosed EIA positive are usually not showing any sign of sickness or disease.EIA may cause abortion in pregnant mares. This may occur at any time during the pregnancy if there is a relapse when the virus enters the blood. Most infected mares will abort, however some give birth to healthy foals. Foals are not necessarily infected.
Coggins Test (for EIA)

The Coggins test (agar immunodiffusion) is a sensitive diagnostic test for equine infectious anemia developed by Dr. Leroy Coggins in the 1970s.
Currently, the USA does not have an eradication program due to the low rate of incidence, however many states require a negative Coggins test for interstate travel. In addition, most horse shows and events require a negative Coggins test. Most countries require a negative test result before allowing an imported horse into the country.
It is recommended to verify that all the horses at a breeding farm and or boarding facility have a negative Coggins test before using their services. A Coggins test should be done on an annual basis. Tests every 6 months are recommended if there is increased traveling.
Currently, the USA does not have an eradication program due to the low rate of incidence, however many states require a negative Coggins test for interstate travel. In addition, most horse shows and events require a negative Coggins test. Most countries require a negative test result before allowing an imported horse into the country.
It is recommended to verify that all the horses at a breeding farm and or boarding facility have a negative Coggins test before using their services. A Coggins test should be done on an annual basis. Tests every 6 months are recommended if there is increased traveling.
Laminitis (Founder)
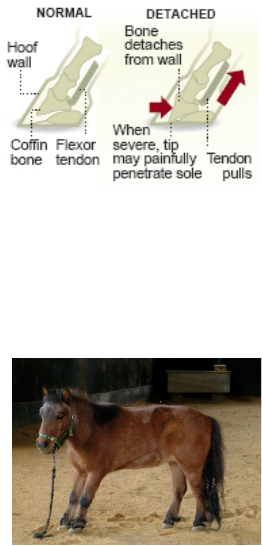
Laminitis is a disease that affects the feet of ungulates. It is best known in horses and cattle. Clinical signs include lameness, inflammation, and increased temperature in the hooves. Laminitis is characterized by inflammation of the digital laminae of the hoof, and severe cases with outwardly visibly clinical signs are known by the colloquial term founder. Laminitis literally means inflammation of the laminae, and while it remains controversial whether this is the primary mechanism of disease, evidence of inflammation occurs very early in some instances of the disease.Laminitis is characterized by a 'compromise in the interaction' of the Laminae between the hoof wall and the coffin bone, the mechanism of which remains unclear and is currently the subject of much research. Laminitis can be either mechanical or systemic
Signs
Signs
- Increased temperature of the wall, sole and/or coronary band of the foot.
- A pounding pulse in the digital palmar artery. (The pulse is very faint or undetectable in a cold horse, readily evident after hard exercise.)
- Anxiety
- Visible trembling
- Increased vital signs and body temperature
- Sweating
- Flared Nostrils
- Walking very tenderly, as if walking on egg shells
- Repeated "easing" of affected feet
- Lameness
- The horse standing in a "founder stance" (the horse will attempt to decrease the load on the affected feet). If it has laminitis in the front hooves, it will bring its hindlegs underneath its body and put its forelegs out in front called "pointing"
- Tendency to lie down, whenever possible or, if extreme, to remain lying down.
Colic
Colic in horses is defined as abdominal pain, but it is a clinical sign rather than a diagnosis. The term colic can encompass all forms of gastrointestinal conditions which cause pain as well as other causes of abdominal pain not involving the gastrointestinal tract. The most common forms of colic are gastrointestinal in nature and are most often related to colonic disturbance. There are a variety of different causes of colic, some of which can prove fatal without surgical intervention. Colic surgery is usually an expensive procedure as it is major abdominal surgery, often with intensive aftercare. Among domesticated horses, colic is the leading cause of premature death. The incidence of colic in the general horse population has been estimated between 10 and 11 percent on an annual basis. It is important that any person who owns or works with horses be able to recognize the signs of colic and determine whether or not a veterinarian should be called.
Signs
Signs
- Pawing and/or scraping
- Stretching
- Frequent attempts to urinate
- Flank watching: turning of the head to watch the stomach and/or hind quarters
- Biting/nipping the stomach
- Pacing
- Repeated flehmen response
- Repeated lying down and rising
- Rolling
- Groaning
- Bruxism
- Excess salivation
- Loss of appetite
- Decreased fecal output
- Increased pulse rate
- Dark mucous membranes
Deworming

Deworming (sometimes known as worming or drenching) is the giving of an anthelmintic drug (a wormer, dewormer, or drench) to an animal to rid it of intestinal parasites, such as roundworm and tapeworm. Purge dewormers for use in livestock are often formulated as a liquid that is squirted into the back of the animal's mouth, as an injectable, or as a pour-on which can be applied to the animal's topline. In horses, purge dewormers are most commonly formulated in an oral paste or gel form, but a liquid drench form is often used by veterinarians. Daily or continuous wormers are also commonly used in horses. Some Types of worms include, Tape worms, Pinworms,Ascarids (large Roundworms),Bots,Large Strongyles (Blood Worms),
Strangles

Strangles (also equine distemper) is a contagious upper respiratory tract infection of horses and other equines caused by a bacterium, Streptococcus equi var equi. Strangles is enzootic in domesticated horses worldwide. The contagious nature of the infection has at times led to limitations on sporting events.Clinical signs include fever, heavy nasal discharge, and swollen or enlarged lymph nodes in the neck and throatlatch. Affected animals may also stop eating and have a dull aspect.
Strangles has a 1% mortality rate. Mortality is lower in cases without complications than it is in cases of bastard strangles. The disease is very contagious and morbidity is high. Precautions to limit the spread of the illness are necessary and those affected are normally isolated. An isolation period of 6 weeks is usually necessary to ensure that the disease is not still incubating before ending the isolation.
Strangles has a 1% mortality rate. Mortality is lower in cases without complications than it is in cases of bastard strangles. The disease is very contagious and morbidity is high. Precautions to limit the spread of the illness are necessary and those affected are normally isolated. An isolation period of 6 weeks is usually necessary to ensure that the disease is not still incubating before ending the isolation.
Potomac Horse Fever
Potomac Horse Fever (PHF) is a potentially-fatal febrile illness affecting horses caused by the intracellular bacterium Neorickettsia risticii. PHF is also known as Shasta River Crud and Equine Monocytic Ehrlichiosis. Signs and symptoms of PHF include acute-onset fever, depression (sometimes profound), inappetance, mild colic-like symptoms, decreased manure production, profuse watery non-fetid diarrhea endotoxemia, edema due to protein imbalances, abortion by pregnant mares, and acute laminitis (20 to 40 percent of cases). Infected horses founder usually within three days of the initial symptoms, thought to be secondary to endotoxemia.Death may occur and is usually due to severe laminitis leading to founder.Horses may not always display any other symptoms beyond a fever.
Other Common Equine Diseases
Some vaccines are considered "core" vaccines that cover diseases that all horses need to be immunized against. Some horses may need to be immunized only when there is significant risk that they will be exposed to the disease in their natural environment, or if they may be exposed when traveling, showing, or competing. In addition, horses must be vaccinated at different life stages. Most vaccines need to be given annually.
Tetanus (lockjaw)
Tetanus is caused by a bacterial toxin normally found in the soil and in the feces of horses. The bacteria that produce the tetanus toxin need a decreased oxygen supply to multiply, so any area where there is a deep puncture wound or where a wound has healed over (such as the navel stump of a newborn foal) is an area where tetanus can thrive. Symptoms of tetanus include a protrusion of the third eyelid and stiff neck, progressing to overall muscle stiffness causing a 'sawhorse' stance. Tetanus is often fatal, but a yearly vaccine can prevent it, and the vaccine is a good idea because small cuts can go unnoticed and become infected.
Equine Encephalomyelitis (sleeping sickness)
This is a disease that affects the nervous system, and can be caused by equine encephalomyelitis viruses (Eastern, Western, and Venezuelan), which are carried by mosquitoes. Signs include depression and a high fever, followed by a period when the horse appears blind, nervous and uncoordinated, with muscle tremors, and eventually, complete paralysis. Proper vaccination and good mosquito control are important to help prevent this disease.
Equine Influenza
This viral disease is spread by inhalation of drops of infective material. Signs include a dry, hacking cough, sudden onset of fever, watery nasal discharge, weakness, loss of appetite and depression. Infection with equine influenza is rarely fatal but can cause problems such as emphysema, pneumonia or bronchitis.
Equine Herpesvirus (rhinopneumonitis, rhino, viral abortion)
There are 2 types of equine herpesvirus: EHV-1, which causes respiratory disease (fever, cough, nasal discharge), reproductive problems (abortion, stillbirth), and neurological problems (hindlimb weakness, difficulty walking, sometimes paralysis); and EHV-4, which is usually limited to respiratory problems. Once a horse has been infected with EHV-1 or EHV-4, he will always be a carrier, and may shed the virus during times of stress.
West Nile Virus
Horses get WNV by being bitten by an infected mosquito; some horses do not show any signs and recover on their own, but in some horses the infection affects the central nervous system and causes signs including fever, weakness or paralysis of the hind limbs, impaired vision, lack of coordination, head pressing, convulsions, inability to swallow, and coma.
Rabies
This is a viral infection of the central nervous system, and although it is not common in horses, rabies can be transmitted to horses by the bite of an infected animal such as a skunk, raccoon, fox, dog or bat. Rabies can be transmitted to people. We recommend that you check with your veterinarian regarding recommendations for rabies vaccination for your horse.
Tetanus (lockjaw)
Tetanus is caused by a bacterial toxin normally found in the soil and in the feces of horses. The bacteria that produce the tetanus toxin need a decreased oxygen supply to multiply, so any area where there is a deep puncture wound or where a wound has healed over (such as the navel stump of a newborn foal) is an area where tetanus can thrive. Symptoms of tetanus include a protrusion of the third eyelid and stiff neck, progressing to overall muscle stiffness causing a 'sawhorse' stance. Tetanus is often fatal, but a yearly vaccine can prevent it, and the vaccine is a good idea because small cuts can go unnoticed and become infected.
Equine Encephalomyelitis (sleeping sickness)
This is a disease that affects the nervous system, and can be caused by equine encephalomyelitis viruses (Eastern, Western, and Venezuelan), which are carried by mosquitoes. Signs include depression and a high fever, followed by a period when the horse appears blind, nervous and uncoordinated, with muscle tremors, and eventually, complete paralysis. Proper vaccination and good mosquito control are important to help prevent this disease.
Equine Influenza
This viral disease is spread by inhalation of drops of infective material. Signs include a dry, hacking cough, sudden onset of fever, watery nasal discharge, weakness, loss of appetite and depression. Infection with equine influenza is rarely fatal but can cause problems such as emphysema, pneumonia or bronchitis.
Equine Herpesvirus (rhinopneumonitis, rhino, viral abortion)
There are 2 types of equine herpesvirus: EHV-1, which causes respiratory disease (fever, cough, nasal discharge), reproductive problems (abortion, stillbirth), and neurological problems (hindlimb weakness, difficulty walking, sometimes paralysis); and EHV-4, which is usually limited to respiratory problems. Once a horse has been infected with EHV-1 or EHV-4, he will always be a carrier, and may shed the virus during times of stress.
West Nile Virus
Horses get WNV by being bitten by an infected mosquito; some horses do not show any signs and recover on their own, but in some horses the infection affects the central nervous system and causes signs including fever, weakness or paralysis of the hind limbs, impaired vision, lack of coordination, head pressing, convulsions, inability to swallow, and coma.
Rabies
This is a viral infection of the central nervous system, and although it is not common in horses, rabies can be transmitted to horses by the bite of an infected animal such as a skunk, raccoon, fox, dog or bat. Rabies can be transmitted to people. We recommend that you check with your veterinarian regarding recommendations for rabies vaccination for your horse.
